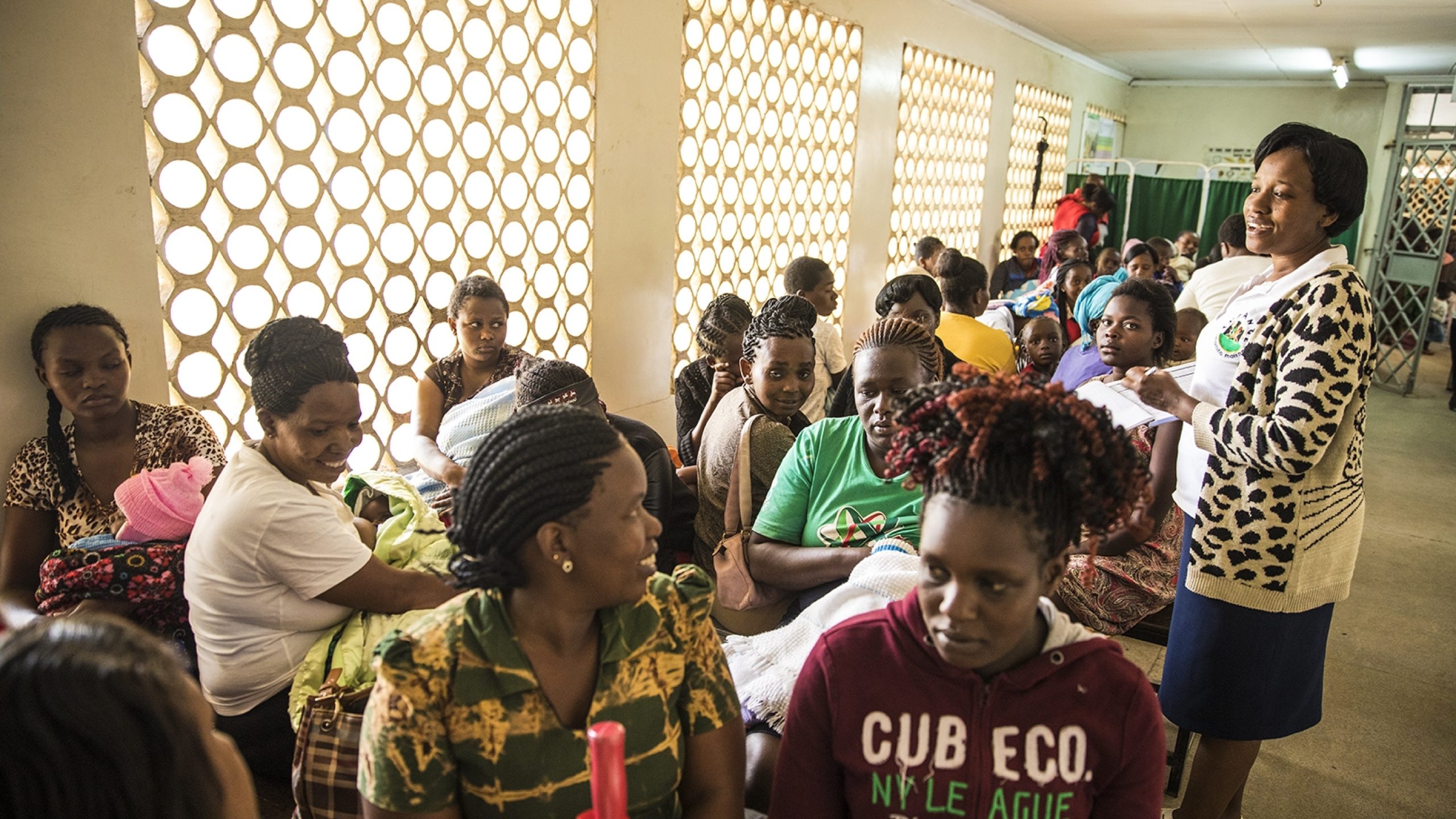The United Nations Office for Project Services (UNOPS)

Delivering for mothers in Nairobi
For the health sector, non-functional infrastructure means patients can’t access health clinics close to their homes, health clinics lose medical supplies that need refrigeration and medical professionals must fight to save lives in overcrowded or unsanitary conditions.
For the estimated 89,000 people who live in Kayole, a low-income area located in Nairobi city’s Eastlands, it’s an all too familiar situation.
Kayole has three public health centres. The Kayole 1 Health Centre is a vital part of the neighbourhood’s health infrastructure and serves approximately 52,000 people.
Many of the women who visit the maternal facilities at Kayole 1 have been referred there by community health volunteers.
Community health volunteers dedicate much of their own time visiting people at home to help raise awareness about health matters, as well as services that are available in the area.
Based on their training, if they believe someone needs to see a medical health professional, they collect basic information and refer them for a clinic visit.
Bernard Karari has served as a community health volunteer for 15 years.




As the only man working in this field in Kayole, he has his work cut out for him.
“Sometimes the men don’t want women to talk to them about some issues so I am the only person who can do it,” he says.
It is important for us to talk to both men and women about these matters. Everyone should understand about health.”
Before maternal facilities at the health centre at Kayole were functional, Bernard experienced a tragic incident helping a woman give birth on the street.
“The lady was hypertensive and we could not think of how to bring her to a hospital as there was no transport. Sadly both she and the baby died from loss of blood,” he recalls.
“I can see that things are much better now,” he adds.

For over two decades, the maternity building at Kayole 1 did not house functioning maternity facilities.
Lilian Muiruri, a nurse and supervisor at the centre says: “Deliveries were not possible here before. Women had to give birth at home or at the local chemists. It was unsafe but these women work as housewives and street vendors. Their husbands are casual labourers. They cannot afford transport at a moment’s notice.”
In support of a United Kingdom’s Department for International Development funded UNICEF project, UNOPS rehabilitated the maternity facilities at Kayole 1. Green technology, such as solar panels, was installed at the centre to help provide a constant source of power. Over 100 community health volunteers were also trained.


Twenty-one year old Adrianna Adembo gave birth to her second baby at the new facilities at Kayole 1. When she had her first child, Cherry, she had to travel to another town much further away to give birth. This time, she could stay much closer to home and return to the clinic easily for health check-ups - both for her newborn son and herself.
Within a month of opening the doors to the much-improved facilities at Kayole 1, the medical staff helped deliver 54 babies. They expect to welcome many more in the future.
About the project
Kenya has some of the highest rates of maternal mortality in the world. According to World Bank data, for every 100,000 live births, approximately 510 women lose their lives during pregnancy and childbirth. To help address this challenge, UNOPS is supporting UNICEF to reduce maternal mortality and strengthen healthcare services across five of the worst affected counties in Kenya.
As part of this $12 million project, funded by the United Kingdom’s Department for International Development, 57 health centres were rehabilitated incorporating a range of green technology retrofits and solar powered solutions, designed to minimize electricity usage and provide access to water services. Close to 500 days of training were provided to community volunteers and health workers, with more than 14,000 people trained. The project was completed in June 2018, with the facilities handed over in the course of 2017 and 2018. The health centres now stand to benefit an estimated 1.6 million people (based on catchment population numbers) across five counties: Garissa, Homabay, Kakamega, Nairobi and Turkana.