The United Nations Office for Project Services (UNOPS)

Inside a Kenyan maternity ward
The third and final part of our series comes from the maternity ward of Turkana’s only referral hospital, full with brand new babies, their mothers and the people who care for them all.
The Lodwar County Referral Hospital in Turkana provides full facilities for maternal care and can handle caesarean sections, premature births and birth-related complications. It is the only referral hospital in Turkana County.
- In a three-part series, we explore the realities of pregnancy and childbirth in one of Kenya’s poorest counties.

Kandi, the nurse in charge of the maternal ward explains that as awareness efforts gained traction among the community, more women travel to Lodwar to seek help.
“We are very happy to see more women and girls [here]. We want them to come in. Only thing is a problem of space,” she tells us.


From approximately 90 deliveries a month at the end of 2016, the hospital now performs nearly 300.
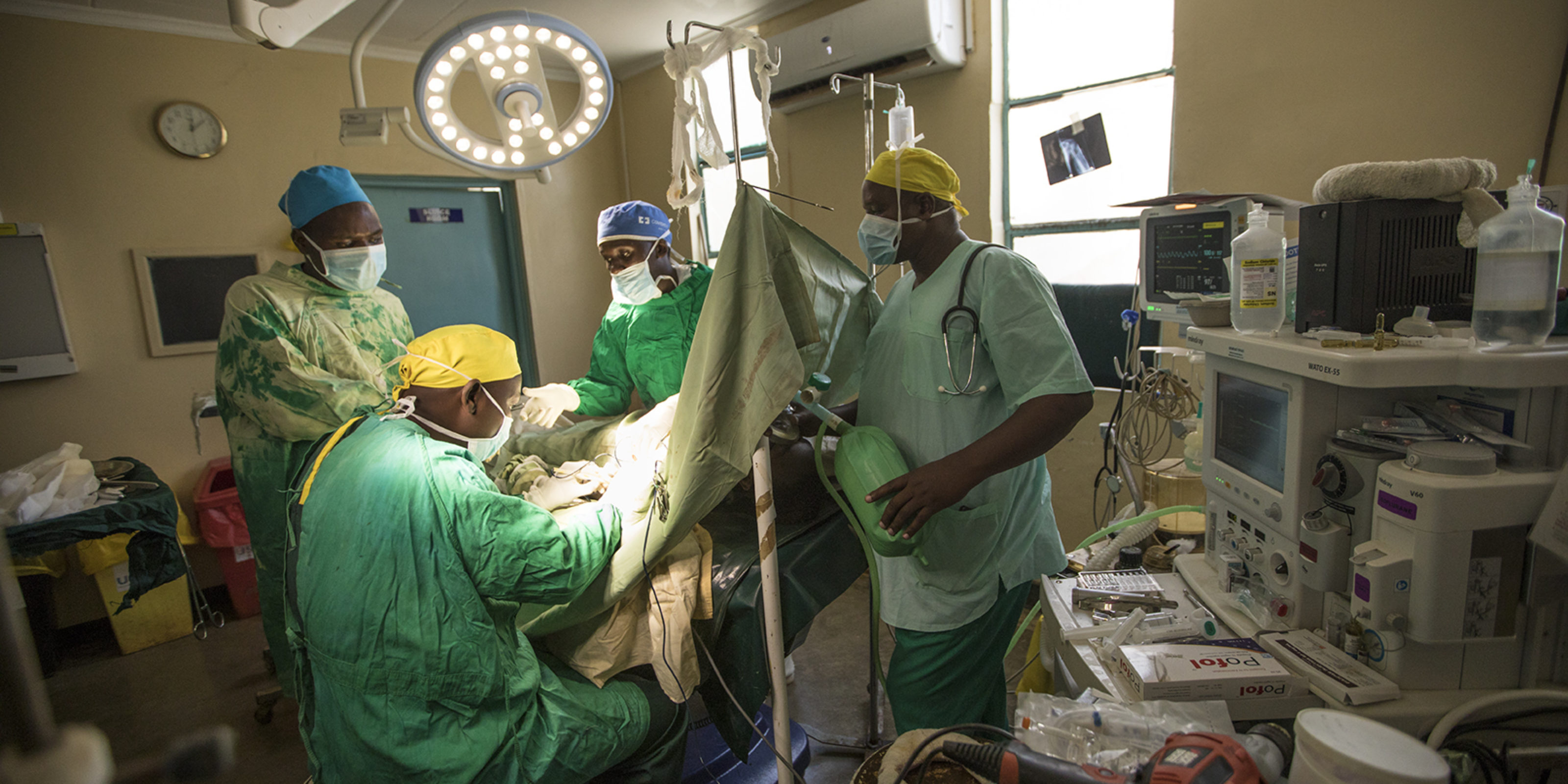
The facility has a post-delivery recovery room and a kangaroo-care room — a space reserved for mothers to care for underweight or premature babies, to help stabilize them. The operating theatre, a common facility, is used for a range of surgeries.
Dr. Gilchrist Lokoel, a surgeon and the hospital’s Chief Executive Officer explains why this is not adequate: “This is the only theatre we had until now and mothers had to give birth in the same place where we do what we call ‘dirty surgeries’ like gunshot wounds. This is not good for anxiety or psychology of the women. It makes them feel like once they go in there, they will not come out again.”
Some women travel from more than 500 kilometres away to reach the facility, a journey which Dr. Gilchrist describes as, “pure hell.”
There are a few ambulances available in the county but the journeys are long and very uncomfortable.
“The woman in labour can be bumping around in the back of the vehicle for ten hours before she reaches us,” he says.
Sitting on one of the ward’s beds is a young woman we had met three days earlier at the smaller Kangatosa health centre. At the time, Anita’s mother had brought her in with what appeared to be labour pains. Anita’s community health volunteer had been there to support and coach her while the health worker checked on her.


Anita has come to the ward in Lodwar because her labour had been complicated and more than the staff in the smaller centre could manage. The staff at Kangatosa feared that Anita may need a caesarean section and called the only ambulance in the area to transport her to the Lodwar Hospital. The distance between the facilities is approximately 45 kilometres by land. She spent four hours in the ambulance, on the heavily potholed road that connects the two places.
“It hurt me a lot. I wanted to get down and lie down again,” she says.
Kandi tells us, “She is okay. We were getting her ready for the operating room, but then she delivered naturally in the night.”
Anita's baby girl will be named by the village elders during a traditional ceremony. A few women from her village are on their way to Lodwar, on foot, to take her back.
In the meantime, nurse Kandi takes it upon herself to coach the new mother on the safest ways to feed and care for her baby.
“We cannot say how old she [Anita] is and she too does not know. But we are helping her to learn some ways of looking after her baby before she goes back,” Kandi explains.



Anita will leave the hospital with a mother-baby pack that, among other small items, includes petroleum jelly and a baby blanket.
Leaders from this hospital believe that one way to support women in the community is to make an effort to get the men more involved in healthcare.
“We go out and talk to people and as Turkana men we talk to other men,” Dr. Gilchrist explains.

“We also use small incentives. In the mother-baby pack, we also put something in for the fathers. We give them a maasai shuka [piece of fabric]. In this Turkana heat, they love it. They wrap themselves in it and go about.”
Dr. Gilchrist and his colleagues believe that they can see the fruits of their efforts, albeit slowly.
“More men agree to hospital deliveries and sometimes we see them here near the woman’s bed.”


About the project:
Kenya has some of the highest rates of maternal mortality in the world. According to World Bank data, for every 100,000 live births, approximately 510 women lose their lives during pregnancy and childbirth. To help address this challenge, UNOPS is supporting the United Nations Children's Fund, to reduce maternal mortality and strengthen healthcare services across five of the worst affected counties in Kenya — Turkana is one of them.
As part of this $12 million project, funded by the United Kingdom’s Department for International Development (DFID), 57 health centres were rehabilitated incorporating a range of green technology retrofits and solar powered solutions, designed to minimize electricity usage and provide access to water services. Close to 500 days of training were provided to community volunteers and health workers, with more than 14,000 people trained.
The project was completed in June 2018 and the facilities were handed over in the course of 2017 and 2018. They now stand to benefit an estimated 1.6 million people (based on catchment population numbers) across the five counties: Garissa, Homabay, Kakamega, Nairobi and Turkana.
UNOPS in Turkana
In Lodwar, the project team renovated the maternity ward at the County Hospital, upgrading the rooms and providing extra space for the women and staff that use the facilities. A new operating theatre has been built exclusively for maternal and infant health-related surgeries.
In Kangatosa, a new maternity ward has been constructed and fitted, with green technology. Funded by DFID's International Climate Fund, this included the installation of solar panels and energy efficient light fixtures enabling this off-grid facility to be fully functional on solar energy.












